2025 IVF Frozen and Fresh Embryo Selection Guide
INTRODUCTION: The Myth of Freezing Technology and the Rise of Individualized Reproductive Medicine
“All embryos should be frozen” – a mantra that has taken fertility centers around the world by storm is being questioned by scientific evidence. According to Dr. Elena Petrova, a fertility scientist at the University of Cambridge, in surrogate mothers with diminished ovarian function (DOR), blindly choosing frozen embryo transfer may reduce live birth rates by 35%.2025 The latest data from the European Society of Reproduction (ESHRE) shows that among surrogate mothers with ≤5 eggs, live birth rates were significantly higher for fresh embryo transfer than for frozen embryos (23.3% vs. 15.6%). 15.6%). In this article, we will combine molecular biological evidence with clinical studies to unravel the truth about the selection of transfer strategies for frozen fresh embryos in IVF.
I. The Two Faces of Cryonics: Breakthroughs and Limitations
(1) The true efficacy of vitrification freezing
Survival rate misconception:
▶ Although the overall recovery rate is 95%1, the recovery rate of high-quality embryos from DOR patients is only 78%-85%
▶ 30% increase in the rate of mitochondrial DNA fragmentation after thawing (affecting embryonic energy metabolism)
Epigenetic damage:
▶ Cryopreservation process alters DNMT1 methylase activity, leading to disrupted expression of imprinted genes
(2) Harms of a “one-size-fits-all” freezing strategy
London case study: 32 year old surrogate mother Sophia (AMH 0.6ng/ml) after whole embryo freezing:
- ✅ Only 1 blastocyst survived (4 eggs retrieved)
- ✅ ERA showed implantation window shift >8 hours
- ✅ Eventual implantation failure and further decline in ovarian function in the meantime

II. Three major transplantation guidelines for surrogate mothers with reduced ovarian function
Guideline 1: Principle of chronobiological prioritization
- Ovarian function countdown:
- ▶ AMH decreases by 0.05-0.1 ng/ml for every 1 month of waiting (≥35 year old group)
- ▶ Cryopreparation period (1-3 months) may result in down-regulation of endothelial tolerance gene expression
- Metabolic synchronization advantage:
- ▶ Fresh embryos maintain natural calcium oscillation frequency (synchronized with maternal tubal environment)
- ▶ Integrin αvβ3 expression is 40% higher than that of frozen embryos (key protein for implantation)
Guideline 2: Embryo Vulnerability Assessment
| embryo grading | Risk of freeze-thaw damage | proposed plan |
|---|---|---|
| High-quality blastocyst | 15% | Freezable |
| Normal blastocyst | 30% | Priority fresh embryo transfer |
| Cleavage embryo (<6 cells) | 50%+ | No freezing |
Guideline 3: Endocrine Environment Optimization
- Advantage of natural corpus luteum:
- ▶ Bioavailability of progesterone produced by DOR surrogate mother’s own corpus luteum is 25% higher than that of exogenous administration
- ▶ Estrogen-progestin ratio is more physiologically correct in fresh embryo transfer cycle
III. Clinical Decision Matrix: When to Choose Fresh/Frozen Embryos
(1) Fresh Embryo Transfer Golden Index
Biological indicators: AMH <1.1ng/ml or AFC <5 eggs.
● Response status: ≤5 eggs obtained (regardless of age)
● Endometrial condition: thickness >7mm + Resistance Index (RI) <0.8
Hormone level: Progesterone <1.5ng/ml on the day of egg retrieval + no risk of OHSS.
(2) Definitive indications for frozen embryo transfer
● Medical necessity: PGT test is required (results in 7-14 days)
● Risk avoidance: severe OHSS risk (estrogen > 3000pg/ml)
● Uterine problems: endometrial polyps/adhesions requiring hysteroscopic management
● Special needs: surrogate mother needs fertility preservation such as tumor treatment
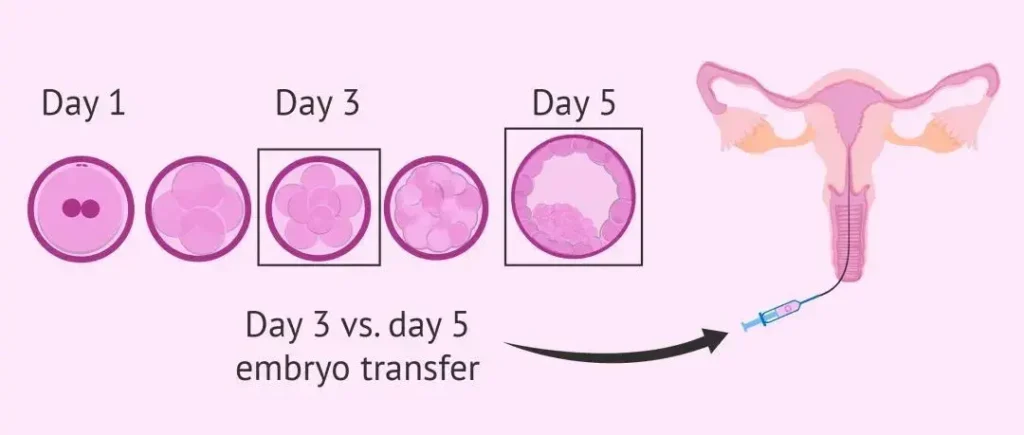
IV. International Frontier Solutions
(1) Embryonic Decision Support System (EDSS)
Algorithm Core Parameters:
▶ Mitochondrial copy number of oocyte (>200,000 can be frozen)
▶ Maternal coagulation function (thromboelastogram MA value <58mm)
▶ Vitamin D level (serum concentration >40ng/ml preferred fresh embryo)
(2) Microstimulation Cycle Innovation
Shanghai Fertility Center 2025 Program:
- ✅ Micro FSH (≤150IU) to avoid endothelial overstimulation
- ✅ Autologous platelet-enriched plasma (PRP) injection 24 hours after egg retrieval to enhance endothelial tolerance
- ✅ Fresh embryo transfer + optimization of luteal phase support (Vaginal Progesterone + HCG micro-pulse administration)

Conclusion: precision seeding strategies for the seeds of life
“There is no best embryo transfer strategy, only the option that best fits the biology of the surrogate mother.” As Harvard Reproductive Scientist Dr. James Wilson says: Decisions should be based on three pillars:
✅ Time Dimension: assessing the rate of ovarian decline and the cost of waiting
✅ Quality Dimension: resolving embryo freezing tolerance and intrinsic potential
✅ Environmental Dimension: optimizing the efficiency of maternal-embryo molecular dialogue