Immune Embryo Implantation Failure Demystified: A Guide to Reconstructing Maternal Immune Tolerance in Surrogate Mothers
Introduction: When Quality Embryos Meet the “Immune Firewall”
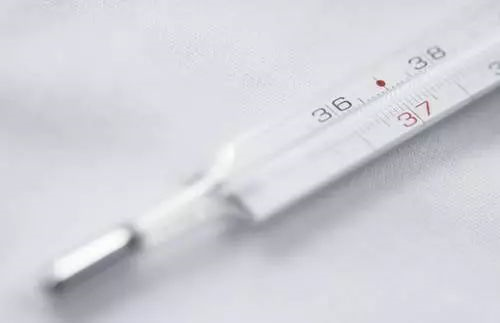
When Sophia Müller (37), a surrogate mother from Berlin, failed to transfer grade AA blastocysts for the third time, her fertility doctor, Dr. James Wilson, presented a devastating statistic: “80% of unexplained implantation failures are associated with maternal-fetal immune dysregulation – your NK cell activity is higher than that of the embryo at risk. Your NK cell activity is 2.3 times higher than the threshold” . This reveals the harsh truth of reproductive medicine: even if the embryo and lining are perfect, the surrogate mother’s maternal immune recognition abnormality may still destroy the seed of life as an “invader”.
I. Embryo implantation: crossing the surrogate mother’s “immune triple hurdle”
As a “half-homozygote” carrying 50% of foreign genes, the nature of embryo implantation is a precise immune negotiation:
(i) Localization period: initiation of immune navigation
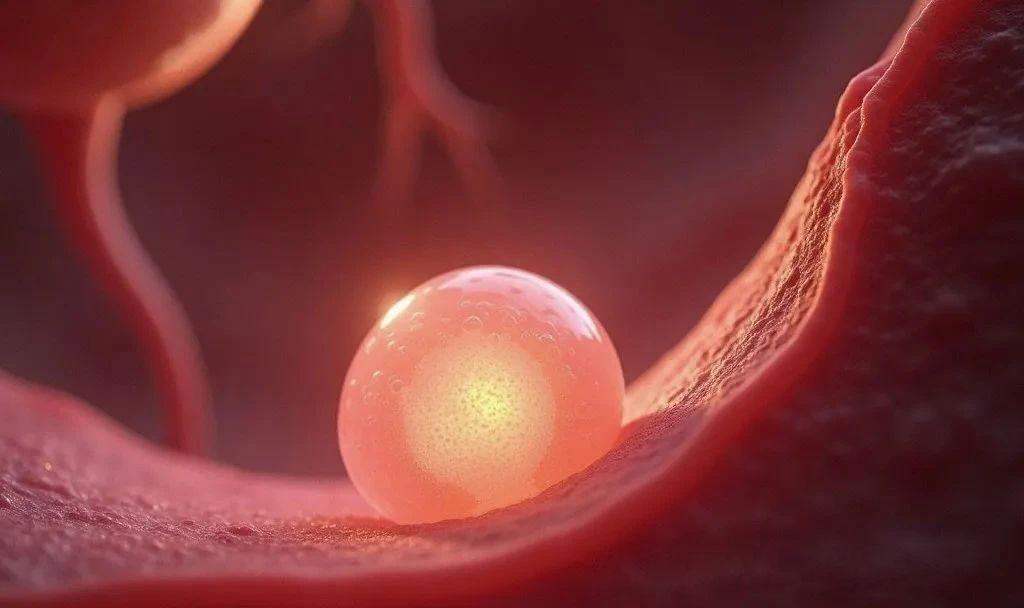
Key event: the embryo breaks through the zona pellucida and searches for the endometrial “landing site”
Immunoregulation:
→ endometrial epithelial cells secrete CXCL12 chemokines, guiding the embryo to direct its movement
→ TGF-β released by immune cells suppresses local inflammatory response
(ii) Adhesion phase: a biomolecular “handshake”.
Core mechanism: integrin αvβ3 binds to bone bridging proteins to form a “molecular glue”
Immune interference:
❌ Positive antiphospholipid antibody: disrupts the spatial structure of adhesion molecules, decreasing the binding efficiency by 40%
❌ Excessive TNF-α: inhibits integrin expression, leading to embryo slippage
(iii) Invasive phase: the ultimate test of immune amnesty
Healthy state: trophoblast cells moderately invade the endothelium assisted by metalloproteinases (MMP-9)
Pathological state:
→ NK cytotoxic granules (perforin/granzymes) attacking the trophoblast
→ Abnormally elevated thromboxane A2 blocking uterine helical arterial remodeling
University of Cambridge study confirms that a successful pregnancy requires that surrogate mothers maternal establishment of an immune-tolerant microenvironment – -that is, down-regulate pro-inflammatory response (Th1), up-regulate anti-inflammatory protection (Th2)
Second, three major immune imbalances: surrogate mother’s mother’s “invisible killers”
Killer 1: NK cell “over-defense”
Data comparison:
| norm | normal range | Repeated Failure of Surrogate Mothers |
|---|---|---|
| Peripheral blood NK cell activity | 7-15% | >18% |
| Endometrial CD56+ cell count | <5% glandular area | >12% |
Clinical Impact: Highly Toxic NK Cells Reduce Implantation Rates from 68% to 19%
Killer 2: HLA Hypercompatibility – The Missing “Identity Code”
Mechanism: When couple’s HLA-II similarity is >65%, surrogate mother fails to produce enough closed antibodies (APCA)
Consequences:
→ trophoblast cells are exposed to macrophage attack
→ placental vascular network formation is blocked, risk of miscarriage increases 3-fold
Killer 3: Th1/Th2 “Inflammatory Storms”
Golden ratio: Th1 (pro-inflammatory): Th2 (anti-inflammatory) should be <10.5 4
Signs of imbalance:
⚠️ IFN-γ >25 pg/mL
⚠️ IL-4 <5 pg/mL
Microenvironmental changes: uterine fluid changes from a “nutrient pool” to “acid bath” (pH drops). Microenvironmental change: uterine fluid changed from a “nutrient pool” to an “acid bath” (pH decreased to below 6.8).
The way to solve the problem: precise immunoregulation program
Program 1: Lymphocyte active immunization (LIT)
Applicable people: closed antibody negative or HLA high compatibility surrogate mothers
Operation process:
A, extraction of paternal lymphocytes –> subcutaneous injection into the surrogate mother’s womb
–> Stimulate APCA antibody production –> Efficacy assessment –> APCA positive conversion: initiate transplantation cycle
B. Extraction of paternal lymphocytes –> Subcutaneous injection into the mother’s body of the surrogate mother –> Stimulation of APCA antibody production –> Evaluation of therapeutic efficacy –> Failure to convert to positive: additional 1-2 immunizations
Clinical data: surrogate mother’s live birth rate increased from 31% to 79% after APCA positive conversion
Option 2: Targeted immunosuppressants
Cyclosporin A:
→ Dose: 2.5-3.5mg/kg/d (activated 7 days before implantation)
→ Action: block NFAT pathway, reduce Th1/Th2 ratio by 40%
Fatty emulsion:
→ 20% fatty emulsion IV drip, twice a week
→ Decrease NK cell activity to safe threshold within 48 hours
Option 3: Endometrial immune microenvironment remodeling
Uterine instillation of G-CSF:
→ 300μg recombinant human granulocyte stimulating factor
→ up-regulation of LIF expression, improve integrin function
Vitamin D3 fortification:
→ surrogate mothers with serum 25(OH)D <30ng/mL, supplement 5000IU daily
→ regulate dendritic cell differentiation, inhibit Th17 over-activation
Fourth, surrogate mother maternal conditioning: from laboratory to life
(I) Nutritional anti-inflammatory formula
| original proposal | daily dose | mechanism of action | Surrogate Mom Friendly Recipes |
|---|---|---|---|
| Omega-3 | 1000mg | Inhibits TNF-α synthesis | Wild salmon 150g/week×3 times |
| Japanese emperor oak | 500mg | Blocking the NF-κB inflammatory pathway | Red Onion Salad + Olive Oil |
| N-Acetylcysteine | 600mg | Reduced NK cytotoxicity particles | Take it with warm water on an empty stomach in the morning |
(ii) Golden rule of behavior modification
Stress Management:
→ Uterine artery RI increases by 0.15 9 when cortisol >14 μg/dL
→ 20 minutes of daily meditation for 8 weeks increases implantation rate by 22%
Exercise Prescription:
→ Pelvic Swing Yoga (15 minutes per day)
→ Improves endometrial blood flow rate by 130
V. Cutting-edge breakthroughs: next-generation technology for immune diagnosis and treatment
(I) Endometrial immuno-mapping analysis
The core of the technology: single-cell sequencing to analyze CD56+ uNK cell subpopulation
Clinical value: differentiate cytotoxic (cNK) and protective (dNK) subtypes, reduce misdiagnosis rate by 90%.
(ii) IL-33/ST2L pathway repair
Mechanism: delivery of ST2L agonists to the endometrium via nanocarriers
Trial data: increased the implantation rate of surrogate mothers with repeated implantation failures from 18% to 54% 5
(iii) Microbiome intervention
Regimen:
→ oral Lactobacillus LC40 (10^9 CFU daily)
→ increase regulatory T-cell percentage and decrease IL-6 levels
Conclusion: reconfiguring immune homeostasis for life
“We finally realized: the embryo needs more than just physical space, it’s a ‘declaration of acceptance’ at the immune level.” Johns Hopkins Reproductive Immunologist Dr. Emily Roberts’ insight reveals the nature of fertility – when a quality embryo meets a perfect lining and still fails, the answer is often hidden in the surrogate mother’s maternal immune microenvironment.
Surrogate Mother Action Checklist:
Mandatory indicators: NK activity/Th1-Th2 ratio/closed antibodies (especially ≥2 failures)
Nutritional basis: serum vitamin D test and intensive supplementation
Technical levers:
→ <35 years: priority LIT treatment
→ ≥38 years: combined uterine G-CSF instillation
Mental contract: join the “Mind-Body Program “Stress Reduction Program (certified by the National Center for Reproductive Health)
The ultimate formula: immune balance = embryo acceptance x inflammation control x microenvironmental remodeling. Each precise adjustment is paving the way for warmer soil for life.